Germany recently passed the Hospital Reform Adjustment Act (Krankenhausreformanpassungsgesetz – KHAG). What does this law mean for hospitals?
At the end of 2024, Germany enacted a highly bureaucratic and centralized hospital reform aimed at closing a large number of small hospitals. It is projected that the number of hospitals will drop from 1,800 to 1,300, a decrease of about 500. Although the federal states are originally responsible for hospital planning, in the future, services will only be reimbursed if uniform federal quality requirements for service groups are met. If these requirements are not met, hospitals’ services will no longer be reimbursed. This represents a paradigm shift in responsibility for hospital planning.
The legislative process under the previous government took place largely without the involvement of hospital associations and practitioners. As a result, many practical problems arose that the KHAG was intended to resolve. No real improvements have been made to ensure the provision of care. On the contrary, further qualitative tightening of standards for service groups was decided upon, and the reimbursement of costs for nursing staff was restricted. The result is more bureaucracy and less efficiency in hospital care.
As part of the KHAG, the previous system for reimbursing nursing staff costs has also been revised. How do you assess these changes?
The proposed new regulations will change how nursing staff costs are reimbursed in hospitals: In the future, nursing staff costs will no longer be linked to occupational groups or areas of practice, but rather to specific, distinct tasks. Specifically, this means that administrative, housekeeping, logistical, and technical tasks performed by nursing staff will no longer be billed through the nursing budget. This complex reimbursement logic greatly complicates daily hospital operations due to the high documentation burden. The financial uncertainty facing hospitals will increase with the new nursing budget regulations.
What adjustments would be necessary to achieve a sustainable increase in efficiency in healthcare?
Over the past decade, healthcare policy has lost sight of the fact that hospitals must operate economically. At the urging of unions and nursing associations, healthcare policy has imposed an increasing number of quantitative staffing requirements, particularly in nursing. These staffing requirements were not determined or established based on evidence. They suggest that only this minimum level of staffing ensures good quality of care for patients. These costly staffing requirements must be eliminated. If hospitals are to bear responsibility for their financial situation, they must also be allowed to decide on the use of cost-intensive staffing resources. This entrepreneurial freedom must be restored to them. It would then also be possible to put healthcare contracts out to bid in individual regions and establish price and quality competition for the provision of hospital services. This would benefit all citizens, who currently have to pay high health insurance premiums to cover high hospital expenses.
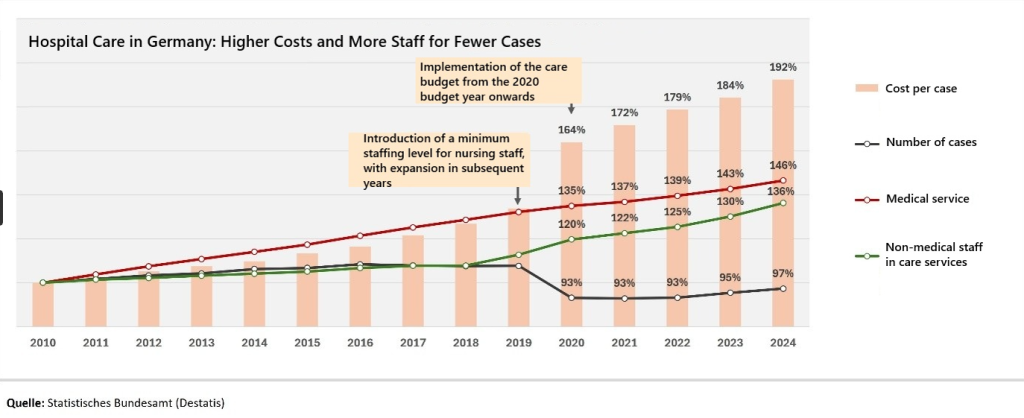
The chart clearly illustrates the spiraling costs that hospitals in Germany are facing.